Pitt Innovation Challenge 2017

Teams competed for funding during the fifth iteration of the PInCh. Projects were awarded a total of $565,000 in funding a the PInCh final event on October 25, 2017. Seven teams competed in a poster session in which event attendees voted for the projects. Six teams then pitched their projects to a live judging panel and audience.
Funds to support this year's challenge were generously provided by DSF Charitable Foundation.

$25,000 Bonus Award Recipient
Team Members: Krista Kutina, DPT, COMT, MS, Michael Boninger, MD, Dave Brienza, PhD, Katee Coleman, Goeran Fiedler, PhD, CPO, Alicia Koontz, PhD, Mary Miknevich, MD, Kristana Mitchell
Description: Mobile gait training system for lower limb amputees that provides real time visual feedback from data derived from an integrated kinetic sensor in the prosthetic limb.

$25,000 Bonus Award Recipient
Team Members: David Rabin, MD, PhD, Greg Siegle, PhD, Kathryn Fantauzzi, MPA, Erik Loraas, MD, Shan Gao, MD, PhD, Demons Mullins, PhD, Ben Kelmendi, Noah Freedman
Description: A novel software platform that taps into existing mobile technology to learn about the user and deliver personalized vibrations to the users' body to enhance performance and resilience in real time.

Team Members: Changfeng Tai, PhD, and William de Groat, PhD
Description: A reversible thermal block technology to suppress or completely disrupt peripheral nerve activity without generating any initial nerve firing.

Team Members: Mioara Manole, MD, Theodore Huppert, PhD, Ervin Sejdic, PhD,and Ericka Fink, MD
Description: Multimodality, non-invasive technology to simultaneously and continuously monitor brain oxygenation and neuronal activity in children after cardiac arrest or other brain injury.

$10,000 Bonus Award Recipient
Team Members: Andrea Sundaram, SHR S/RST, PhD student, Josh Brown, Joshua Chung, SHR S/RST, Rory Cooper PhD, and James Landis
Description: A system to help manual wheelchair users to learn and remember to do adequate pressure reliefs to prevent the development of pressure ulcers.

Team Members: Sandra Sobel, MD, Dave Rometo, MD, Kristine Ruppert, Dr. PH, Linda Siminerio, RN, PhD, Patrick McCarthy, RN, CDE, UPMC
Description: A protocol using continuous glucose monitors for temporary intensive insulin therapy at time of type 2 diabetes diagnosis to induce beta cell restoration and diabetes remission.

Team Members: Ulka Sachdev, MD, Shiyi Shen, Yi Zhu, Michele Morris
Description: Smart compression stocking for patients suffering from chronic venous insufficiency that is adjustable and self-monitoring to reduce symptoms and improve quality of life.

Team Members: Kevin Bell, PhD, William Clark, PhD, Elizabeth Schlenk, PhD, RN, Michael Schneider, DC, PhD, and Gwendolyn Sowa, MD, PhD
Description: Wearable technology-based behavioral intervention that assess activities of daily living and actively informs a customized treatment plan to prevent chronic low back pain.

Team Members: Elizabeth Katrancha, DNP, CCNS, RN, CNE, Joe Lindsay, and Eunice Yang, PhD
Description: Wearable technology that assesses individualized heart rate variability data to predict and warn a person of orthostatic hypotension before it happens to prevent a potential fall.

$10,000 Bonus Award Recipient
Team Members: Ameya Nanivadekar, Santosh Chandrasekaran, PhD, Lee Fisher, PhD, Max Novelli, and David Weir
Description: Universal haptic package is a wearable for upper or lower limb prostheses that will sensorize prostheses and interface with existing and future stimulation systems to provide life-like sensory feedback to the wearer.
Team Members: George Stetten, MD, PhD, and Roberta Klatzky, PhD
Description: New wearable technology patented by the Univ. of Pittsburgh replaces eye motion with finger motion, allowing visually impaired users to scan the environment, rapidly finding and identifying objects by means of computer vision algorithms as communicated through vibratory as well as audio channels.
Team Members: Amit Sethi, PhD, OTR/L, Ervin Sejdic, PhD, John Riley, MBA, and William Clark, PhD
Description: I-HITS is an individualized hand improvement and tracking system, which allows patients with stroke to monitor their hand movement and enables therapists to deliver treatment outside therapy.
Team Members: Mingui Sun, PhD, Wenyan Jia, PhD, and Patrick Strollo, MD
Description: Smart textile wearable device that delivers controlled electrical and vibrational stimulations to lower extremities for treatment of restless leg syndrome.
This year, we incentivized solutions that impact US military veterans through a system of veteran impact bonus awards. Eligible projects received up to an additional $25,000 in bonus awards.
Application Details:
- Explain the impact the project will have on veterans.
- Use an additional 25 seconds at the end of your application video to explain why your solution will impact Veteran’s Health.
- Eligible projects may propose budgets up to $125,000.
- Projects not selected for this bonus award will be eligible for up to $100,000.
“Approximately 235,000 veterans, including roughly 37,400 post-9/11 veterans, live in Southwest Pennsylvania, a region that includes Allegheny County (of which Pittsburgh is the county seat) and twelve other surrounding counties. A dense community of veterans lives in the urban area of Pittsburgh, while others are dispersed in the region’s more rural counties. Veterans comprise between 9 and 12 percent of each county’s total population, a rate that is higher than the national average of 6.7 percent, making Southwest Pennsylvania one of the densest veterans communities in the nation.” Reference.
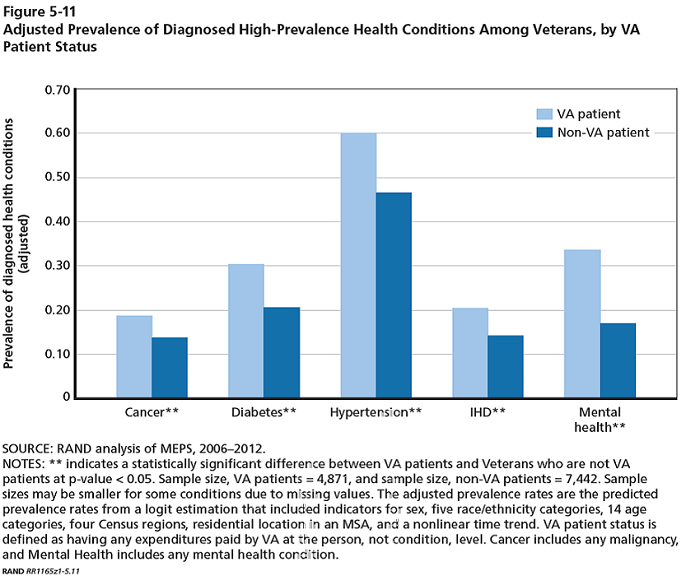
Determining which health problems have more impact on veterans is complicated. The Veterans Administration (VA) health system provides care to some veterans, but not all. Veterans who have access to VA health system are prioritized and tend to be more ill than veterans who do not have priority for care in the VA system. The difference in prevalence between VA patients and veterans not eligible for VA services provides an indication of which health conditions impact veterans in significant ways.
In 2015, RAND completed a study titled “Current and Projected Characteristics and Unique Health Care Needs of the Patient Population Served by the Department of Veterans Affairs”
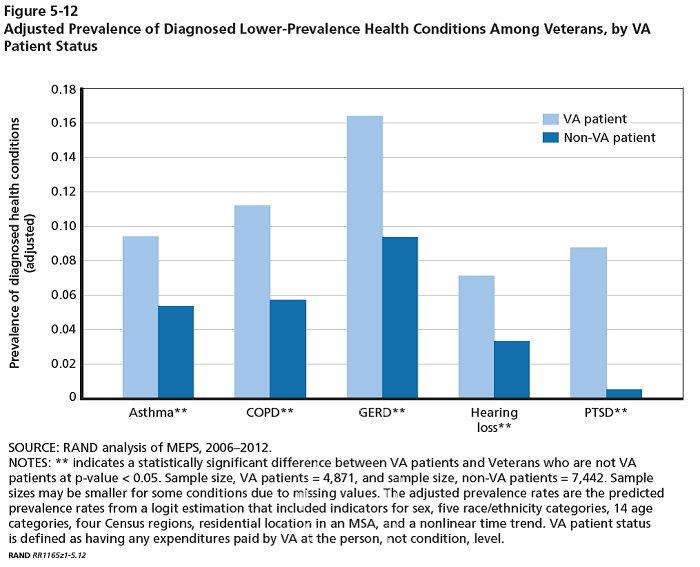
The charts below highlight the differences in prevalence for different health conditions. They highlight conditions that are more prevalent in general (Figure 5-11) and less prevalent in general (Figure 5-12). The largest relative differences are in the less prevalent conditions (Figure 5-12). It is reasonable to assume that because more severe health problems make a veteran more likely eligible for VA services, the ratio between the prevalence among VA patients and prevalence among non-VA patients is a way to estimate which conditions differentially impact veterans in important ways. Thus PTSD, COPD, hearing loss, Asthma and GERD are conditions that specifically impact veterans